|
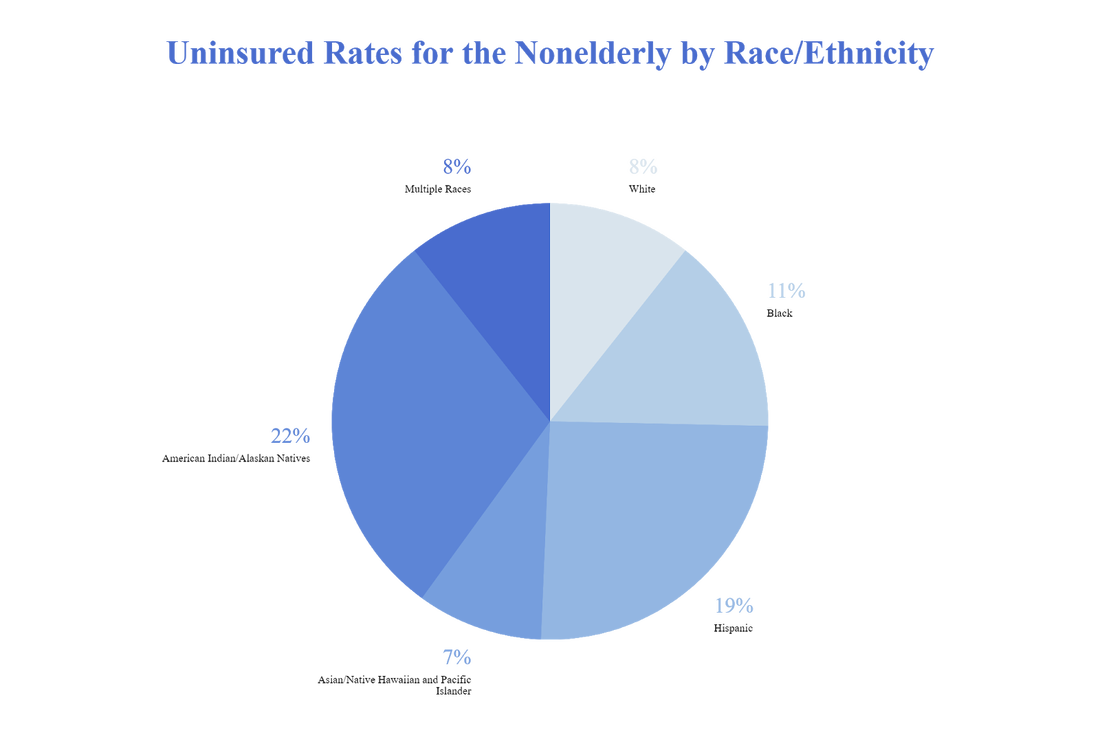
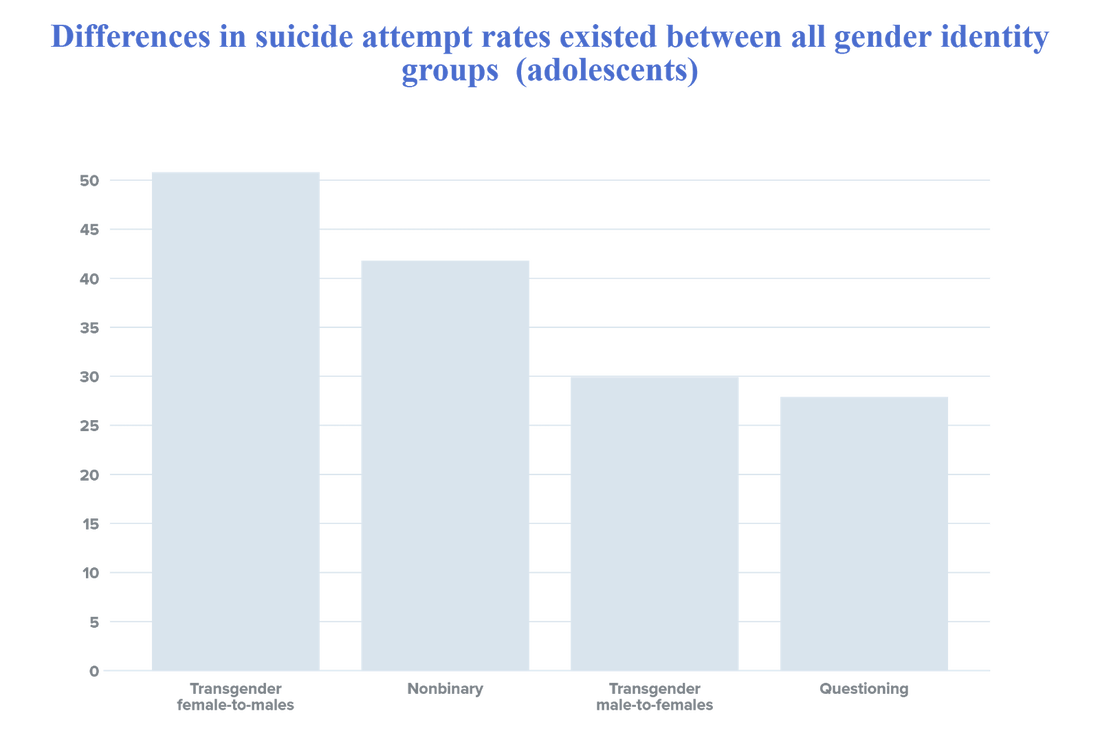
Hi Everyone! Today, we, Keshika Vasuja and Archi Das Gupta from HealthNeedsRx, will be discussing disparities in mental health care especially concerning racial, gender, and sexual minorities. It is extremely essential to spread awareness about Mental Health Disparities to prevent minority groups from suffering. Racial/ethnic, gender, and sexual minorities often suffer from poor mental health outcomes due to multiple factors including inaccessibility of high-quality mental health care services, the cultural stigma surrounding mental health care, discrimination, and overall lack of awareness about mental health. As individuals across the U.S. grapple with illness, the death of loved ones and the ripple effects of social isolation, the mental health system is struggling to meet the increased demand for mental health services. What is most striking, however, is the disparate impact on Black, Indigenous and Latinx communities. These disparities and barriers to mental health care not only violate the professional values of the counselling profession but also constrain the ability of counsellors to provide mental health care in high need communities on par with other health care professionals. It is vital to increase access to mental health care for our most vulnerable populations and address the disparities in who receives services. AFRICAN AMERICANS: * Rates of mental illnesses in African Americans are similar to those of the general population. However, disparities exist regarding mental health care services. * African Americans often receive poorer quality of care and lack access to culturally competent care. * Only one-in-three African Americans who need mental health care receive it. * Compared with non-Hispanic whites, African Americans with any mental illness have lower rates of any mental health service use including prescriptions medications and outpatient services, but higher use of inpatient services. * Compared with whites, African Americans are: – Less likely to receive guideline-consistent care – Less frequently included in research – More likely to use emergency rooms or primary care (rather than mental health specialists). * Black people with mental health conditions, particularly schizophrenia, bipolar disorders, and other psychoses are more likely to be incarcerated than people of other races. Barriers to care Despite recent efforts to improve mental health services for African Americans and other minority groups, barriers remain regarding access to and quality of care. The barriers include: • Stigma associated with mental illness • Distrust of the healthcare system • Lack of providers from diverse racial/ethnic backgrounds • Lack of culturally competent providers • Lack of insurance, underinsurance ASIAN AMERICANS/PACIFIC ISLANDERS Cultural barriers include: * Several cultural and structural barriers prevent AA/ PIs from accessing mental health services. * These include the following: * The myth of the model minority—racial/ethnic minority group perceived to achieve a higher degree of socioeconomic success than the population average—creates an unreasonable pressure on people to meet societal and familial expectations leading to poor mental health well-being. * Lack of understanding about mental health and associated stigma, especially among first-general immigrant AA/PIs lead to denial or neglect of mental health issues. Often mental illness is considered a weakness and source of shame/burden among the community. Structural barriers include: • Lack of cultural competency among service providers may lead to misdiagnosis and underdiagnosis of mental health problems for the AA/PIs. • Insufficient multilingual services in the healthcare system makes it difficult for AA/PIs to access mental health treatment. • Lack of or insufficient health insurance, immigration status and high cost of mental health services increase challenges for A/PIs to seek mental health treatment Some other challenges: • Lack of accurate data, evaluation, and research on AA/PIs. • Lack of appropriate intervention strategies for diverse AA/PI populations (including the integration of mental health and primary health care services). • Lack of involvement of AA/PI individuals and family members HISPANICS/LATINOS Mental Health, Utilization of Services, and Disparities: • U.S.-born Hispanics report higher rates for most psychiatric disorders than Hispanic immigrants. • Studies have shown that older Hispanic adults and Hispanic youth are especially vulnerable to psychological stresses associated with immigration and acculturation. • Approximately 1 in 10 Hispanics with a mental disorder use mental health services from a general health care provider, while only 1 in 20 receive such services from a mental health specialist. • Hispanics are more likely to report poor communication with their health provider. Several studies have found that bilingual patients are evaluated differently when interviewed in English as opposed to Spanish and that Hispanics are more frequently undertreated. • Nationally, 21.1% of Hispanics are uninsured, compared with 7.5% of White Non-Hispanic Americans. Low rates of insurance coverage for Hispanic is likely to be a function of ethnicity, immigration status, and citizenship status. Disparities in Hispanic/Latino Children and Adolescents • Hispanic children and adolescents are at significant risk for mental health problems, and in many cases at greater risk than white children. • Among Hispanic students in grades 9-12 in 2015: 18.9% had seriously considered attempting suicide, 15.7% had made a plan to attempt suicide, 11.3% had attempted suicide, and 4.1% had made a suicide attempt that resulted in an injury, poisoning, or overdose that required medical attention. These rates were consistently higher in Hispanic students than in white and black students. • In 2014, Hispanic and white adolescents aged 12-17 in the U.S. were more likely than black or Asian adolescents to have initiated alcohol use or cigarette use in the past year. About 10% of white and Hispanic adolescents initiated alcohol use, compared with 7.3% for blacks and 4.7% for Asian. Approximately 3.9% of Hispanic adolescents initiated cigarette use, compared Past Year Mental Health Treatment, by Race/Ethnicity psychiatry.org 2017 with 3.5% for white adolescents, 2.2% for black adolescents, and 1.5% for Asian adolescents. Barriers to Accessing Mental Health Care • Lack of insurance or inadequate insurance • Lack of knowledge/awareness about mental health problems and services available • Cultural stigma associated with mental illness • Language • Lack of culturally tailored services and culturally competent mental health professionals • Shortage of bilingual or linguistically trained mental health professionals • Difficulties recognizing incipient signs of mental illness No matter how far we have come in terms of innovations in the healthcare field, discrimination and disparities still reign free in the profession. Research has found that there are racial, gender, sexual orientation disparities in healthcare indicatively mental health disparities. But discrimination isn’t the only factor holding minorities back from getting the help they need, another constituent includes being uninsured. The cultural stigma surrounding mental health is another constituent as there are cultural, religious, and spiritual beliefs about mental health in certain minorities. The American Indian and Alaskan Native are reported to have higher rates of mental illness than the rest of the US population. The AI/AN makes up 5.2 million Americans which is only 2 % of the population, which makes them the smallest minority group in America. The reason behind these high rates is because of intergenerational historical trauma linked with the removal of their tribes from their land and the government separating children from their parents to send them to boarding school. These factors led AI/AN to develop PTSD (post-traumatic stress disorder), suicide, anxiety, depression, attachment disorder, and substance abuse. Furthermore, about 33% of American Indian and Alaskan Natives are uninsured which means the majority of them rely on Indian Health Services for healthcare. Other barriers preventing AI/AN from getting help are lack of awareness, service, a distrust with healthcare providers, and the stigma surrounding mental health. The history of oppression and trauma made the natives aloof to modern approaches to mental health. According to the Gallup Poll, about 4.5% of Americans are LGBTQ+ and it is proven that lgbtq+ people are more 2.5 times more likely to have gone through the adversities of depression, anxiety, and substance abuse. People who are LGBTQ+ often experience these adversities because of many constituents such as their community rejecting them and who they are as a person. Another constituent is if they don’t live in a place where there isn’t a large LGBTQ+ population in their particular region, they can often isolated and different from others, especially bisexual people. Though LGBTQ+ people are more likely to seek out and use healthcare services, they often face stigma and discrimination. Due to these factors often refrain or delay getting the healthcare they deserve. In addition, transgender people are more likely to commit suicide than any other sexuality mainly because of the possible physical, emotional, and sexual abuse they endure. It doesn’t help that the Transgender community also faces discrimination from their healthcare professionals. The specific risk factors for LGBTQ+ parental psychological abuse, mistreatment, past suicide attempts, family history of depression, and anxiety. (Toomey, Ph.D., 2020) There are many mental health disparities between genders (male and female). Every year, 1 out of 5 women in the US contain some sort of mental health problem. These mental problems can range from PTSD, depression, anxiety, and an eating disorder. Depression being the most common as twice as many women experience depression. The risk factors for women include the wage gap, socioeconomic disadvantages, victims of violence, and women being primary caregivers which means they spend more money and time allocating care than male caregivers. Furthermore, women often experience work overload as they work at home and their workplace and women face sexual and physical abuse more. In addition WHO stated that women and men are treated differently when they seek mental health services even when they display the same symptoms and test scores. There are numerous barriers for women who seek mental health services such as lack of insurance, awareness, time, and intervention strategies.
In order to battle these disparities, mental health workers should be more aware of their impact if they aren’t already. They should treat men and women equally and focus on the physical perspective of mental illness by paying attention to the symptoms. Healthcare workers should consider screening patients for particular disorders and mental health illnesses. In addition, the fight for healthcare to be more accessible and offer high-quality health care. Moreover effectuating mental health services that are both ethnically and linguistically adept are crucial to many minority groups such as American Indians and Alaskan Indians. This goal can be achieved by funding for healthcare training and hiring diverse health care staff. Also increasing awareness for mental health in minority groups and destigmatize mental illnesses. Citations: Psychiatric Association, American. “Mental Health Disparities: American Indians and Alaska Natives.” Mental Health Disparities: Diverse Populations, 2017, www.psychiatry.org/psychiatrists/cultural-competency/education/mental-health-facts Toomey, Ph.D., R., 2020. Risk And Protective Factors For Suicide Among Adolescents: A Look At Gender Identity And Sexual Orientation. [online] American Foundation for Suicide Prevention. (Uninsured Rates for the Nonelderly by Race/Ethnicity, 2020) (American Indian & Alaskan Native Mental Health — NoStigmas, 2020)
0 Comments
Leave a Reply. |
Welcome to our blog, Medquity!Here we will post extra articles on health disparities to display the profound health inequities in our healthcare system. These are updated every other weekend, so check back regularly! Archives
July 2021
CategoriesHealthNeedsRx ©
Copyright 2021 |
 RSS Feed
RSS Feed
